The second-year nursing master’s student is starting to feel the pressure. Her patient has broken out into a rash all over his body and he’s past due for his medications. The harsh beeping sound of an electrocardiogram pings through the air as the patient bellows coughs in quick succession.
Moving quickly, the student conducts a head-to-toe examination of the patient, administers the overdue medications and checks his vital signs to determine a course of action. More lights, more sounds, more coughing until suddenly…
A message flashes across the screen: “Simulation complete.” The student, relieved, takes off her headset.
Simulating realistic patient care was considered the stuff of science fiction as recently as a few years ago. At the Marquette College of Nursing, an institution long viewed by its peers as a technology leader, that new simulation reality has just arrived.
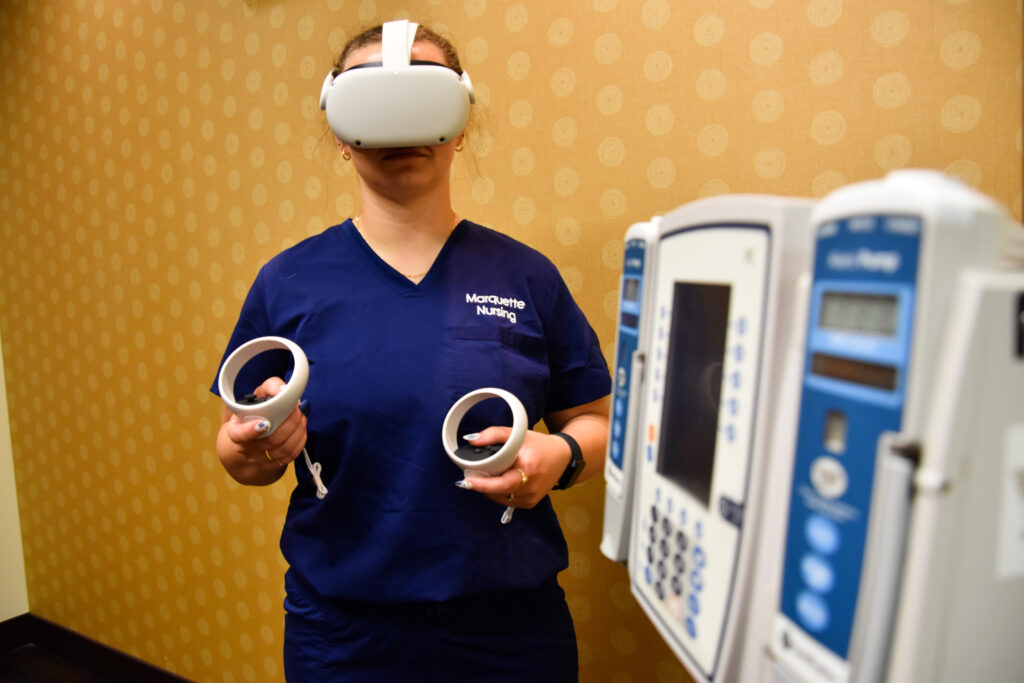
The College of Nursing is piloting immersive virtual reality simulation, or IVRS, with a cohort of students for the first time this fall. Oxford Medical Simulation, the college’s partner for virtual reality, provides realistic scenarios that mirror real-world health care experiences. Nursing students are using Meta Quest 2 virtual reality goggles to bring these experiences to life, inhabiting a computer-generated environment that is as close as one can get to a hospital without being in it.
“Their complete awareness is in this virtual room,” says Anne Costello, the director of the Wheaton Franciscan Healthcare Center for Clinical Simulation. “There’s a 360-degree experience in the headset with sound and other sensory feedback. You really are transported to that simulation environment.”
For decades, nursing students honed their craft on mannequins that have a built-in array of human processes, such as realistic pulses and breathing. The College of Nursing has a selection of these mannequins that simulate different patient demographics and health conditions, part of an effort that has established Marquette as a clinical simulation leader. As Marquette prepares for an expanded and modernized physical simulation center in the college’s future home, virtual reality presents an opportunity to complement traditional simulation techniques, engaging more students.
And although instructors can operate mannequins remotely and even speak through them, virtual reality takes patient interaction to new levels, allowing students to revisit scenarios multiple times while expanding the range of available patient scenarios.
While virtual reality gaming experiences have been possible for some time, health care simulation is an emerging technology that has rapidly developed from prototypes into a usable patient care scenario. “When I first tried the product that we’re using, I said to myself, ‘OK, this seems like it’s ready for the open market,” says clinical instructor Amanda Potter.
Nursing professor Dr. Kristina Thomas Dreifuerst is on the forefront of the IVRS revolution. Together with researchers from around the country, including lead investigator Dr. Cynthia Bradley from the University of Minnesota, Dreifuerst is working on a pilot program to integrate IVRS with clinical preceptorships and thorough debriefings. The project, which is funded through a $1.3 million grant from the American Nurses Foundation’s Reimagining Nursing Initiative, will give nurse educators around the country better guidance on how to implement virtual environments in their own classrooms.
Dreifuerst, who has also led other simulation-related innovations that benefit students and faculty, sees the technology as necessary to prepare future nurses for the stressors of a hospital environment.
“We were finding that employers’ expectations of new graduate nurses didn’t always meet the reality of the current educational model,” Dreifuerst says. “With IVRS, students can have simulation experiences that better prepare them for the complexity of health care.”
Marquette Nursing has set an ambitious target of training 5,000 new nurses in the next decade, part of a broad campaign to help tackle the nationwide nursing shortage. The incoming freshman Class of 2023 is roughly 25 percent larger than the class that came before it.
Admitting more students means a need for more of everything else: building space, faculty, resources and clinical time, to name a few. The college has made substantial investments in solving some of those challenges, including the ongoing renovation of David A. Straz, Jr., Hall, which will become the college’s new 100,000-square-foot home in the summer of 2024. And the college can start clearing hurdles even before the new building opens. Implementation of IVRS helps tremendously on the clinical experience front.
“We are competing for a limited number of clinical sites that will take our students and we’re also up against this challenge of getting students the clinical time they need to graduate. That’s where simulation comes in,” Costello says.
Costello does not see traditional hospital clinicals going anywhere; rather, she views simulations as a necessary supplement to them.
“It’s important to run as many controlled scenarios as we can to expose students to things they’re going to see all the time so when they get in those clinical scenarios, they’re better prepared for it,” Costello says. “This is just one more tool we can use to support our nursing education.”
Marquette Nursing has always been on the front line of nursing education trends, helping to shape the profession’s future. Through piloting IVRS in the nursing program, the college will evaluate how Marquette students can hone their skills in the virtual world to deliver better patient outcomes in the real world.




