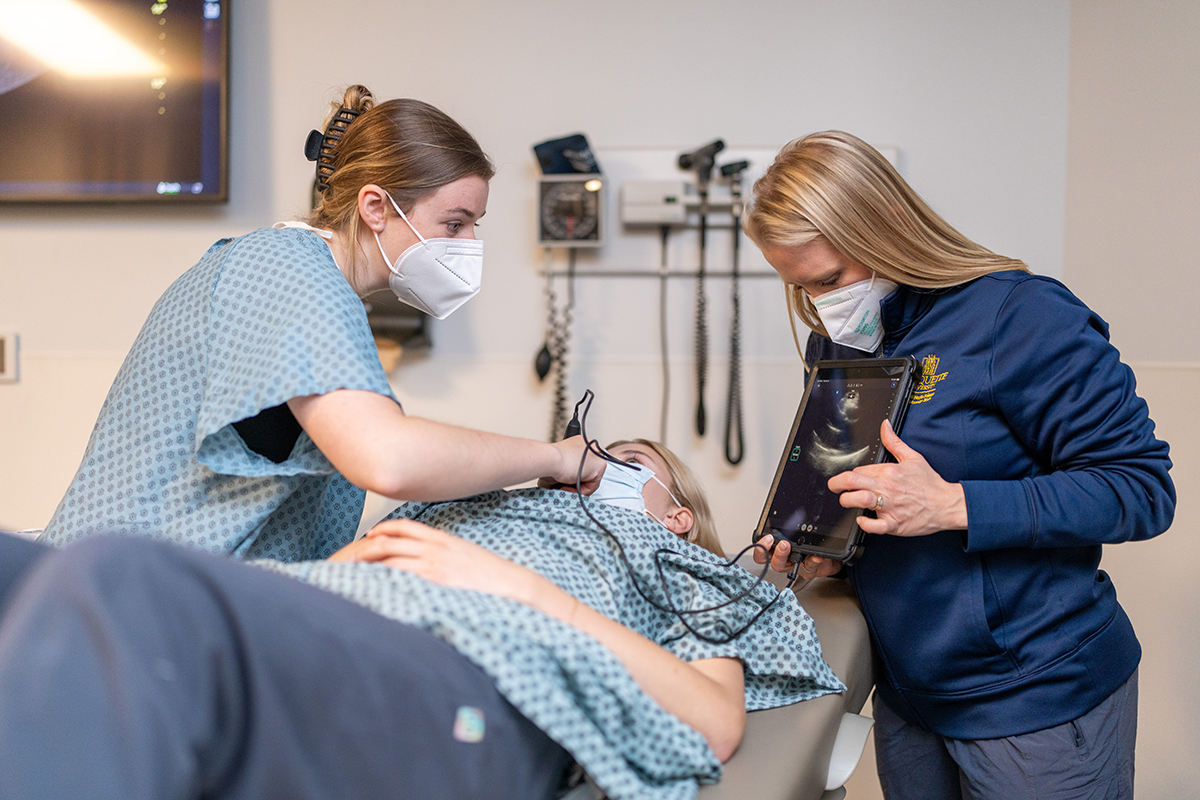
As portable ultrasound devices emerge as a key asset in patient diagnostics, the Physician Assistant Studies program leads the way in teaching this technology

By Sarah Wells, photos by Patrick Manning
Amie Billstrom is no stranger to providing medical care under pressure. Before joining Marquette in 2020 as a clinical assistant professor in the Physician Assistant Studies program, Billstrom provided emergency medical care to patients in mountainous regions of Central America through the U.S. Joint Command’s Operation Central Skies.
When staff or access to technology was limited, Billstrom could always rely on a pocket-sized piece of technology to help her make a life-saving diagnosis — a point-of-care ultrasound device. These portable devices, known by the acronym POCUS, are transformative for health care because clinicians can use them to make quick bedside diagnostic assessments on their own, rather than having to wait for specialized technicians to operate large scanning machines. And now, Billstrom is part of an initiative at Marquette to bring this technology into the hands of new PAs like never before.
Instead of learning about POCUS only in clinical and emergency medicine courses at the end of their program, future PAs at Marquette are now introduced to the technology from day one, making this one of the first PA programs to incorporate ultrasound technology throughout its curriculum. “POCUS is being integrated into a lot of medical school programs and is frequently called a ‘new age stethoscope,’” Billstrom says. “We want to stay on par with these colleagues.”
Mary Jo Wiemiller, department chair and Physician Assistant Studies program director, says that incorporating more portable ultrasound device use into the PA curriculum is an exciting innovation that should serve students far beyond their studies. “This curriculum will hopefully make POCUS second nature in clinical practice,” Wiemiller says. “Our hope is that Marquette PA students can lead the way among other learners for point of care ultrasound use.”
When you think of ultrasound, the first images that likely come to mind are the fetal ultrasounds done periodically throughout a pregnancy to measure developmental progress. Yet, the uses for POCUS devices have expanded in recent years, Billstrom says, extending their relevance to many other clinical situations as well, such as identifying fluid in a patient’s lungs or evaluating heart function.
Additionally, POCUS devices can be used repeatedly without exposing patients to radiation, as an X-ray or CT scan would. “It uses sound waves,” Billstrom says. “It’s low risk to put a probe on a patient.”
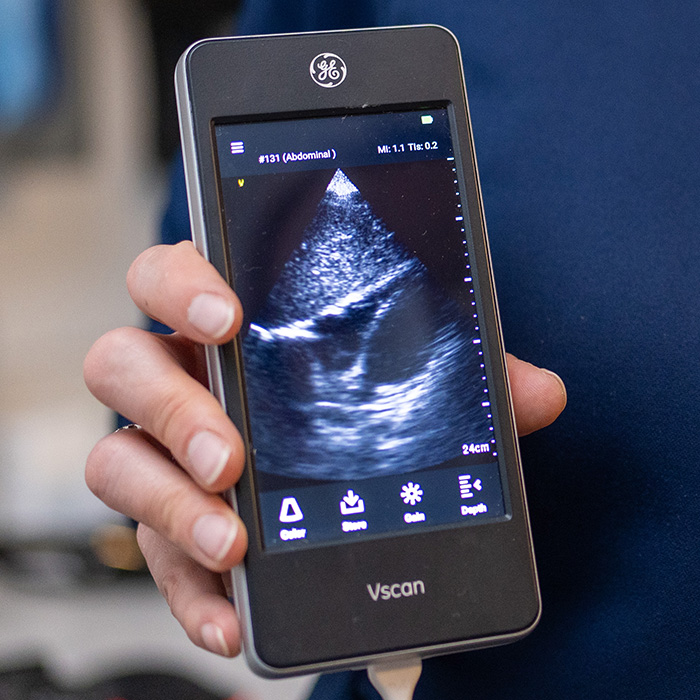
Ultrasound probes can come in many different shapes and sizes, but Billstrom often opts for a portable POCUS that looks more like an electric razor than a complex medical tool. Regardless of their shape, POCUS devices are designed to operate in two different modes: high frequency for evaluating superficial structures like the lungs, and low frequency for deeper evaluations, such as within the abdomen.
In both cases, “echoes” of these ultrasound waves bounce back when they hit something in the body, such as tissue or bone. To make sense of these echoes, clinicians are trained to interpret feedback-formed images on a screen or attached tablet. Understanding how these often grainy images correspond to a patient’s anatomy is one of the steeper learning curves for POCUS, says third-year PA student Liz Horn.
“Things on an ultrasound do not look like they do in textbooks,” says Horn. “It requires a lot of focus, good technique, and a lot of overall consolidation of my medical knowledge to be able to discern what I am looking at.”
Horn says that prior to Marquette’s PA program she’d had few interactions with POCUS, but she has now seen how the technology can be an incredibly important tool across medical specialties. This appreciation is something Billstrom hopes all PA students will take away from the new ultrasound curriculum, as they receive lessons on POCUS use in each semester starting in their first semester in conjunction with their gross anatomy course.
“This curriculum is built longitudinally so that they start very generically looking at anatomy using POCUS alongside their anatomy and physical exam course,” Billstrom says. “Then in their clinical medicine and clinical decision making, we would use POCUS to look at particular patients who have a chief complaint, for example shortness of breath.”
The goal is for students to be more comfortable using POCUS to diagnose pathologies by the time they enter their clinical years, so that they can use a POCUS just as easily as any other diagnostic tool. “Ultrasound has been such a growing field, especially during the COVID pandemic,” Billstrom says. “As we’re putting students out into the workforce to be primary care providers and emergency medicine PAs, they need to know this technology. If they’re only getting on-the-job training, they’re behind the curve.”